She Treated Breast Cancer Every Day. Then She Became the Patient.
By: Aryana Hadjimohammadi“I’m not grateful I got cancer, but cancer made me grateful for many things.”
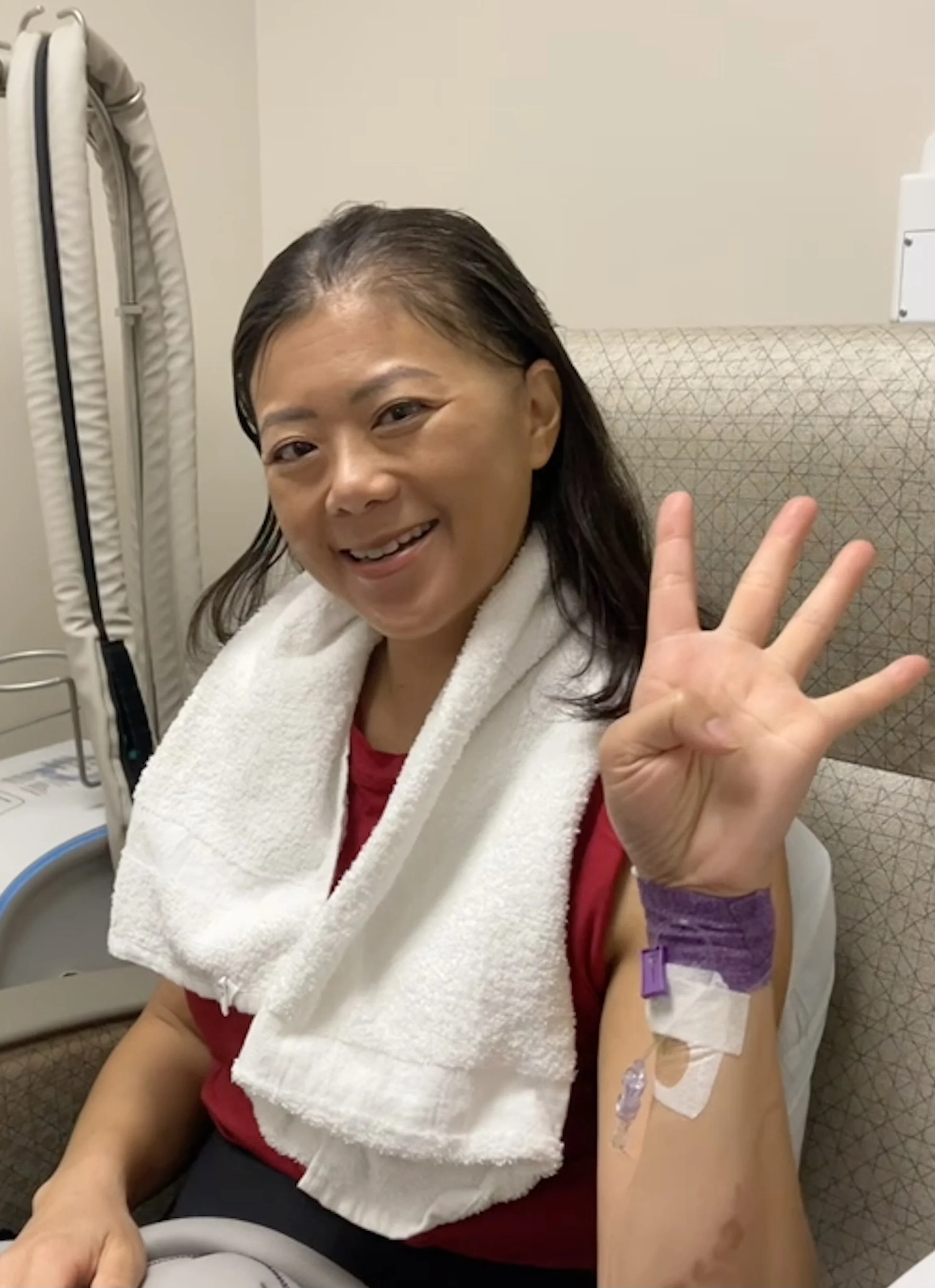
Dr. Sue Hwang is a radiation oncologist. She leads breast radiation oncology at the AdventHealth Cancer Institute. She is also a breast cancer survivor. She is thriving now. But getting here was not easy.
This is her story. And it starts with a routine mammogram.
How she found it
In January 2024, she went in for a routine mammogram. She did this every January, like clockwork.
"I didn't feel anything in my breast," she says. "I was feeling great."
Her friend was the radiologist. He saw calcifications. In her mind, she was not quite panicked. Calcifications, if they are cancer, tend to mean very early-stage disease.
Then they did an ultrasound.
That is when he saw five masses in her breast, as well as an abnormal lymph node.
She was 46 years old.
The shock was not that she got cancer
One in eight women will get breast cancer. She never thought she was above that.
But she was in “complete and utter shock. “I wasn't shocked because I got diagnosed with breast cancer. What shocked me was really the extent that they found in the breast."
She does this job every single day. She knows what characteristics on imaging tend to indicate more aggressive cancers.
Imaging initially showed five suspicious masses in her right breast, but after surgery, doctors discovered more than 10 individual tumors clustered together, stretching across about 11 centimeters of tissue. Combined with cancer in a nearby lymph node, she was found to have locally advanced disease.
The cancer was invasive lobular carcinoma.
"Lobular cancers tend to have this presentation where they're a little bit sneakier," she explains. "You do the mammogram, and the mammogram actually doesn't look that bad, and then you go to the MRI, and the MRI can show more extensive disease."
"If you look at my path report, they stopped counting tumors after 10," she says. "It just said more than 10 tumors."
Three kids. Three different conversations.
Dr. Sue Hwang and her three kids.
Hwang is a single mom. At the time, her children were 11, 13, and 15. Her 13-year-old and 15-year-old had friends whose mothers died of metastatic cancer within the past year.
When it came time to tell them, she decided to tell each of them individually because they all process information differently.
She told her 15-year-old while he was driving on his learner's permit.
"I felt like it felt safe when he's driving the car," she says. "I just knew there was something else to distract him from having a complete breakdown, which, in retrospect, was probably not the best decision."
His first question was, "Are you going to die?"
"No, this is different," she told him.
From there, he shifted. "He was like, okay, what's the treatment like? How are we going to treat this?"
Her 13-year-old had a different response.
"When I was telling him, he pulled out his phone and I thought he was texting his friend," Hwang recalls. "I thought to myself I'm telling you I have cancer, and you're texting your friend. But it turns out he was actually on his phone doing math."
She had always told him: if you want to make your mom feel better, just do your homework. Every night she would say it.
"He had a very interesting response," she says. "I thought it was very sweet that when I'm telling him I have cancer, he pulls out his phone and is like, okay, let me start doing my homework."
Her youngest, 11, had recently started asking heavy questions about death. Not because of her diagnosis. He was just getting curious.
After she told him, he started tracking her. He needed to know where she was, who she was with, when she would be home.
"I think that was just his response," Hwang says. "There's a scary diagnosis going on. But if I know exactly where my mom is and where she is at all times, then everything's better."
The treatment
Hwang's treatment was bilateral mastectomies with immediate reconstruction, then four cycles of chemotherapy, then 16 fractions of radiation, then endocrine therapy and a pill called Verzenio, which is a CDK4/6 inhibitor.
She will be on Verzenio for two years. Her two years will be up in four months. "Very surreal,” she says. The endocrine therapy she will be on for probably another eight years.
Every treatment phase had a hardest part.
Surgery: Not moving.
After mastectomy with implants, the plastic surgeon was very specific. No movement of the chest wall for the first week. Every time you move, you rub the implant against the skin, which delays the recovery process and increases the risk that the implant can fail.
"For me, not moving is really hard," Hwang says. "I'm a single mom with three kids. I'm used to running around. I'm used to folding laundry, cleaning. Going from all of that to all of a sudden being confined to a recliner is very challenging."
She was good at not moving for the first three days. She stayed in her recliner and binge-watched Handmaid's Tale.
Then, on day four, she went for a walk to see manatees. A few days later, she went on a hike.
"I will fully admit I was not a good patient in that respect," she says.
Chemo: The hair loss.
As a doctor, she used to watch patients cry about losing their hair. Part of her would think, look, you need the treatment. The hair will grow back.
Then she became the patient.
"Cancer strips away so much from you when you go through treatment," she says. "They take your breasts, which is obviously a huge part of what makes you a woman. Then all of a sudden, cancer is going to take your hair too. You're just like, are you kidding me?"
She tried cold capping to preserve her hair. It did not work. Her hair is so thick that the cold could not get down to her scalp.
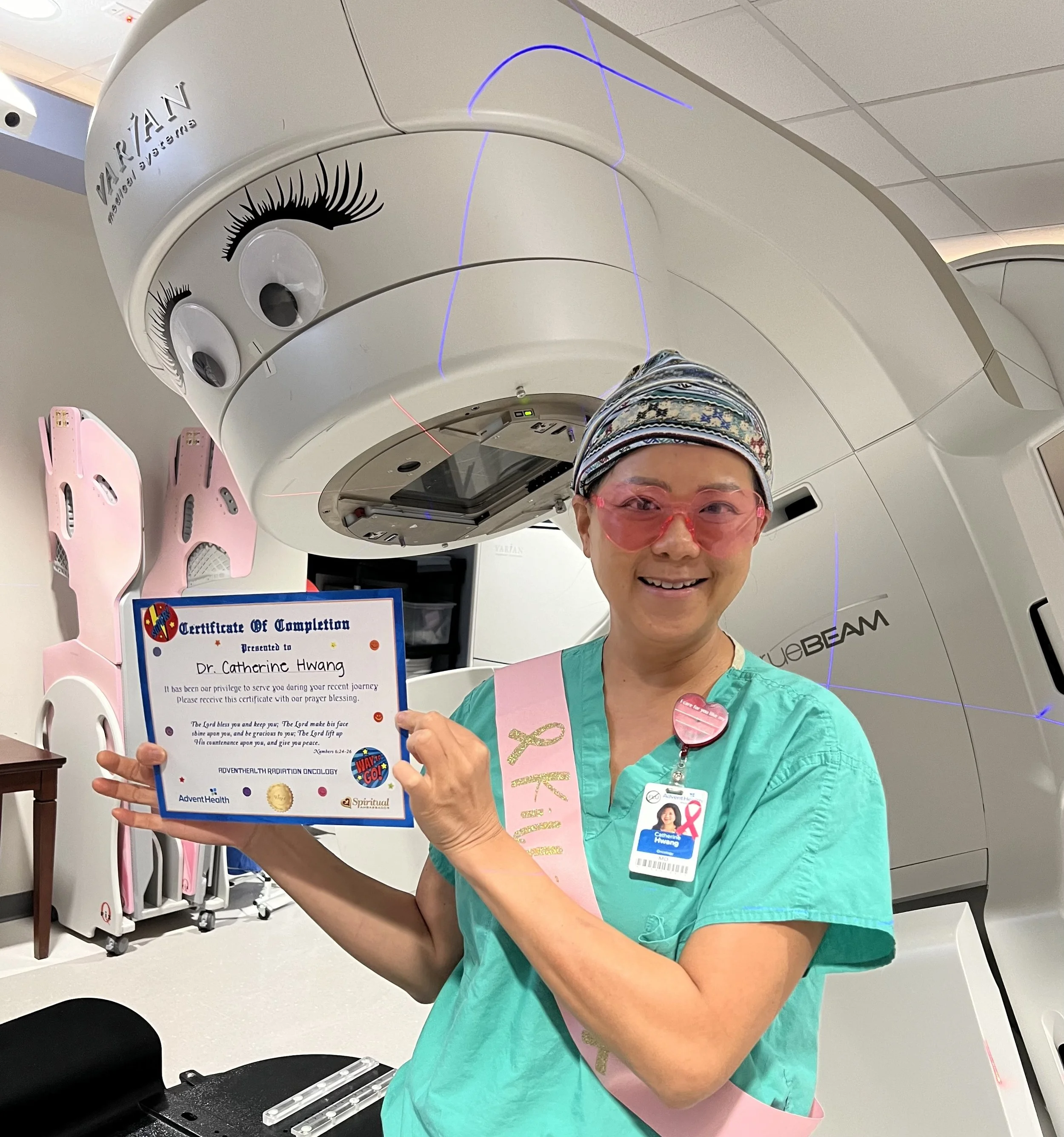
Radiation: Treating patients while being treated.
Hwang did not stop working. Her job wanted her to take more time off. But mentally, working kept her sane.
"When everything around you is changing, if you can do things that you used to do, that is what helps you stay sane," she says. "But in my case, what keeps me sane is also what I'm being treated for."
She was treated at her own center, by her own staff. In the beginning, she worried about making them uncomfortable. They had to see her topless.
"The challenging thing about treatment itself was just the fact that I was doing it while I continued to work," she says. "It's a little bit of a mind game. Trying to counsel people through something that you're actually going through yourself and trying not to see yourself in every patient that you are treating."
When the doctor becomes the patient
Hwang initially tried to keep her diagnosis private. She started coming to work in scrubs and a scrub cap, which was a dramatic change from the business casual attire she normally wore. But she changed her attire to scrubs so that she could wear a scrub cap to obscure her thinning hair.
Then her sideburns fell out. Even with the scrub cap on, it was really obvious. That is when she started telling patients.
"When patients found out, there was just kind of a stop in the conversation," she remembers. "They see doctors as the healthy ones. This doesn't happen to doctors. Then they realize, oh my God, you're just like one of us."
That connection changed everything.
"They know that I have been where they are going," she says. "It makes me a lot more trustworthy. You're not just a doctor anymore. It's the sisterhood of breast cancer patients."
What she learned
Before her own diagnosis, Hwang thought stage correlated with fear. Stage zero? You are going to do fine. Stage four? Of course you are hysterical.
She does not think that anymore.
"Stage does definitely not correlate with fear," she says. "Whether you're stage zero or stage four, when you get told you have this diagnosis, all of a sudden you have to realize, wait, my body didn't do a good job of fixing itself. Wait, I have something that could potentially kill me. It doesn't matter how good your outcome is. Just the word cancer itself is very scary."
She also learned that she cannot do it all. Before cancer, she was the person who said no to help. A meal train? No thanks. She could just order Uber Eats every night for her kids. She did not want people to go through the effort of making her a meal when they had stuff to do.
"What I realized is, the meal train is just people's way of showing you that they care," she says. "Yes, it is an effort for them to get a meal and bring it to you. But when you're sick and you're not feeling great, just that simple act is how they support you."
How her practice changed
After her experience, Hwang completely changed how she talks to patients about life after treatment.
Before cancer, her post-treatment advice was pretty vague. Go for your mammograms. Come for your follow-ups. Eat less, exercise more.
That was about it.
"I didn't really get educated on it," she admits. "In training, we're so focused on treating the cancer. The aftermath was not a priority. It consisted of mammograms and if the mammogram is okay, then the patient’s okay."
Now she is more informative.
"I'm much more specific about recommendations for how to prevent future cancers," she says. "Getting 150 minutes of exercise a week. Two of those sessions should be weightlifting. From a nutrition perspective, you're going to cut out added sugar. You want to cut out alcohol or minimize it. You want to eat a diet high in fruits and vegetables. You want clean proteins. You want good carbs. You want to get out ultra processed foods. You want to sleep eight hours. You want to figure out ways to minimize stress." She also stopped equating being thin with being healthy.
The hardest part came after treatment
“Survivorship, to me, is learning how to live again after the diagnosis, and learning how to live well.”
This is the part Hwang wants every patient and every doctor to understand.
She thought the goal was to get through treatment and get back to life as she knew it. But recovery surprised her.
"When I wake up in the morning, I literally feel like the wicked witch from Snow White," she says. "I walk to the bathroom hunched over because my bones hurt so badly.”
She is on endocrine therapy. For breast cancer patients, 80% are recommended endocrine therapy because they are hormone receptor positive. This medication suppresses the effect of estrogen and sends patients into menopause with side effects, including hot flashes, bone pain, weight gain, mood changes, fatigue, and joint pain.
Before her own diagnosis, she admits she was nonchalant about these side effects. Every woman goes through menopause, she used to think.
"I can't believe I was just so nonchalant with patients," she says.
She is now pushing for better survivorship care. Once active treatment ends, patients often get less follow-up. But that is when things can get hard.
What she wants you to know
If you are newly diagnosed: You will get through it. Find a team you trust. You are in control of your care.
"Patients really need to realize that they do hold power," Hwang says. "They have to know what questions to ask. I would recommend at least a little self-education before they see the doctor so that when they are at the appointment, some of what they’re saying makes a little bit more sense to you. It's kind of like the first time you hear a different language, when you have no idea what is being said. But then as you start to hear it more, it becomes more understandable."
Think you have a symptom? Know the 12 signs.
Dr. Hwang advises watching for changes in your breasts. But sometimes, medical words can be hard to remember or recognize.
That is why Know Your Lemons created a simple, visual way to learn the 12 signs of breast cancer — from a lump to skin dimpling to nipple changes.
If you notice any of these signs, do not ignore it. If you are young and a provider tells you not to worry, get another opinion. Dr. Hwang has seen this happen too many times.
"We are seeing a rise in breast cancer in younger women," she says. "It's really disheartening when you hear these stories of a 30-year-old who felt something in the breast. They went to see a healthcare provider. They get told, 'Don't worry about that. You're too young to have breast cancer.' Then a year later, they get diagnosed with breast cancer, and it's the same mass that they were feeling."
Download the free Know Your Lemons app. It includes a doctor-patient conversation guide to help you advocate for yourself at your next appointment.
If you are at average risk: Hwang recommends that average risk women start mammograms at age 40, once a year. For those with a family history of breast cancer, she advises starting 10 years before the age that family member was diagnosed.
What Dr. Hwang Thinks About Know Your Lemons
Hwang believes that education saves lives, and that is why she supports the work of Know Your Lemons.
“Know Your Lemons is a wonderful organization that empowers women to take control of their health and be aware of the signs and symptoms of breast cancer. They break down complex medical information into information that is easy to understand and adopt.”
She says one thing that stood out to her about the foundation is how it uses simple visuals to reach people everywhere. "One thing that stood out to me about the Know Your Lemons Foundation is how it uses simple, visual images of lemons to explain breast cancer signs in a way that's easy to understand," she says. "This makes important health information accessible to people of different ages, languages, and education levels around the world."
She is also a fan of the Know Your Lemons app, which won best health and fitness app last year, beating Apple Fitness. Asked if she thinks it should be awarded again, she says, "Absolutely."
Her favorite feature is the visual breast self-exam guide. "My favorite feature is the visual breast self‑exam guide, because it shows symptoms clearly instead of relying on medical words," she says. "I also like how the app is available in multiple languages, making it useful for people all over the world."
The Booby Fairy
One of her best friends created a character called the Booby Fairy before Hwang's surgery. Wings, a wand, all pink, blowing bubbles.
"As you're about to head into one of the scariest days of your life, it was just a nice distraction," Hwang says. "From when I got diagnosed to when I saw my friend, that was the first time that I truly laughed in days. It felt so good."
"Laughter is the best medicine," she says. "Crying isn't getting us anywhere, and laughing is actually really good for us."
From Both Sides of the Curtain
Dr. Hwang wrote a book called From Both Sides of the Curtain. Even though she had no interest in becoming an author, she found writing to be cathartic and extremely helpful as she processed her diagnosis. But she also wrote it for patients. She wanted them to know that they are not alone in what they are experiencing. She hears from so many people who apologize for feeling scared and concerned. They do not want to come across as too emotional. So, she wrote the book to say: Hey, I have been taking care of breast cancer patients for 18 years. And when I got the diagnosis, I was terrified. This is me with all my knowledge. So of course, if you are someone who does not deal with breast cancer every day, you are going to be scared.
““I want people to know I got through it. They will get through it too.””
Her story and yours
Dr. Hwang's cancer was not found because she felt a lump. It was found because she went in for her routine mammogram. She did it every January like clockwork. But mammograms do not catch everything, and not everyone has access to them.
That is where breast awareness comes in – knowing what is normal for your body, noticing changes, speaking up when something feels off. Dr. Hwang put it simply: "You are in control of your care."
At Know Your Lemons, we believe that control starts with information. The 12 signs of breast cancer — from a lump to skin dimpling to nipple changes — are things you can learn in two minutes. Things you can check for yourself. Things you can share with the people you love.
Let our app help you learn the signs, do your self-checks, get your mammogram when it is time. And if something does not feel right, do not let anyone tell you are too young, too healthy or too busy.
As Dr. Hwang said, "If you see something and you feel something, and you are not getting the answer that you think you deserve, then you need to go get another opinion."
That is breast awareness. That is early detection. And that is how we save lives.
Resources
Know Your Lemons – Learn the 12 signs of breast cancer
Keep A Breast Foundation – Self-check app and prevention resources
From Both Sides of the Curtain by Dr. Sue Hwang – Available wherever books are sold
Breast Cancer 101 — Keep A Breast — Plain-language breast cancer education
American Cancer Society — Screening Guidelines — Current recommendations on when and how to screen
National Breast Cancer Foundation — Resources from early detection through survivorship
FORCE: Facing Our Risk of Cancer Empowered — For those with hereditary breast cancer risk
Young Survival Coalition — Support for young women diagnosed with breast cancer